The symptoms of hereditary spastic paraplegia vary widely among patients and even within families in terms of symptoms and age of onset. Muscle weakness and stiffness, cramps, or spasms are commonly observed, making walking difficult and increasing the risk of falls. Reflexes in the lower limbs are generally greatly increased (hyperreflexia).
Symptoms of Spastic Paraplegia
These symptoms are accompanied by extreme physical fatigue.
In some patients the signs worsen over time, while in others they may disappear after adolescence. In 10% of cases, patients have eye problems, intellectual deficits, loss of muscle control, or deafness due to brain damage.
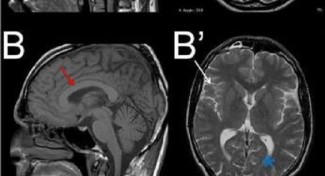
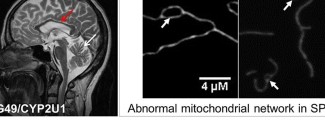
Patients with spastic paraplegia may present symptoms suggestive of other neurodegenerative diseases such as amyotrophic lateral sclerosis or cerebellar ataxia. An MRI scan of the brain or spinal cord, which records electrical signals in the brain or muscles, can help with diagnosis. Genetic testing can often confirm the disease by identifying a genetic mutation.
At Paris Brain Institute
Our researchers are working on projects aimed at developing diagnostic tools and identifying the genes responsible for the variability observed between patients.
Through collaborative work involving the genotyping-sequencing core facility at Paris Brain Institute, Giovanni Stevanin’s team has developed a diagnostic kit capable of sequencing all genes known to be involved in hereditary spastic paraplegia in just a few hours and with a high degree of reliability. The development of this kit represents a considerable time saving and a major advance in the molecular diagnosis of these diseases. This kit is distributed nationally and internationally.
A study conducted by Prof. Alexandra Durr has led to the discovery of factors influencing the age of onset of hereditary spastic paraplegia type 4.These initial results are very important in the search for modifiers of hereditary spastic paraplegia type 4 and open up new avenues of research into the impact of mutation and gender on the age of onset and the severity of the disease.
Researchers in this team have also investigated the existence of a potential link between spastic paraplegia type 7 and cerebellar ataxia. A number of patients with spastic paraplegia also present symptoms of cerebellar ataxia, which are only diagnosed retrospectively. The results of this research could enable earlier diagnosis and treatment of patients.
Khalid H. El Hachimi and his team have shown similarities in nervous system damage between spastic paraplegia type 11 and amyotrophic lateral sclerosis. This discovery will enable clinicians to make an accurate and early diagnosis of “atypical” ALS by testing for mutations in the SPG11 gene. Furthermore, understanding the mechanisms involved in these diseases paves the way for the development of new targeted therapies.