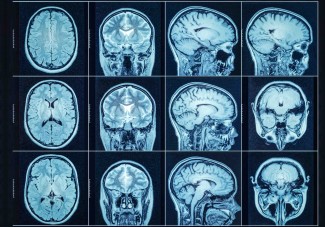
Can brain imaging reveal whether a person is affected by depression? This question has driven research for many years. Changes in brain structure have indeed been observed in patients with depression, suggesting that structural MRI might one day help physicians better understand and diagnose this disease. As part of an international collaboration between teams from the Institute for Molecular Bioscience (IMB) at the University of Queensland in Australia, the Paris Brain Institute, and Bicêtre Hospital in Paris, researchers put this hypothesis to the test. They show that MRI scans of grey matter provide useful clues, but in no way constitute a diagnostic tool. Their findings are published in Translational Psychiatry.
Although it is one of the leading causes of disability[1] worldwide, depression remains poorly understood, perhaps because of its heterogeneous presentation and the influence of multiple factors on its onset—such as genetics, stress, trauma, and physical health. Previous studies have shown a reduction in hippocampal volume in people with depression or a greater frontal cortical thickness in patients who respond well to antidepressant treatment.
“These clues suggest that certain brain regions are involved in the onset of depression, but also in the progression of depressive episodes and in treatment response,” explains Baptiste Couvy-Duchesne (Inria), a researcher in the Aramis team at the Paris Brain Institute, currently seconded to QIMR Berghofer in Brisbane, Australia, and senior author of the study. “We wanted to determine whether depression could be diagnosed using imaging, particularly structural MRI, which allows us to analyze the architecture of gray matter—the tissue composed of neuronal cell bodies and dendrites .”
Computers trained to read the brain
The international team, formed through the collaboration between the Paris Brain Institute and the University of Queensland, analysed brain MRI scans from nearly 8,000 individuals recorded in the UK Biobank, around 1,500 of whom had a history of major depressive disorder. Using advanced computational models, the researchers trained algorithms on tiny three-dimensional units called voxels—the 3D equivalent of pixels—derived from the database images. The goal was to determine whether imaging markers could identify individuals affected by depression.
One of their models, based on a machine-learning approach, performed better than chance: individuals who were truly depressed were more likely to obtain a higher predictive score for depression risk.
“Our results indicate that grey-matter structure does indeed contain information related to depression,” explains Jiayue-Clara Jiang, a researcher at the Institute for Molecular Bioscience (IMB) at the University of Queensland and first author of the study. “However, this information remains limited. Brain structure alone is not sufficient to diagnose the disorder accurately.”
Another interesting finding: a more complex approach based on deep learning—often considered one of the most advanced methods in artificial intelligence—did not yield better results.
A complex disorder with multiple causes
Depression does not have a single biological cause. Supporting this idea, the team found that predictions based on imaging partly overlapped with genetic risk for depression. When these two sources of information were combined, predictions improved slightly—but not enough to be clinically useful.
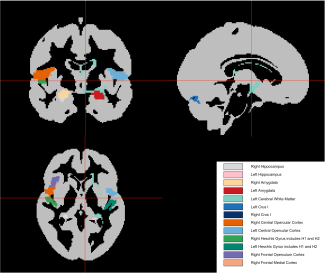
The researchers also examined which brain regions contributed most to accurate predictions. They found that the hippocampus and amygdala, which are associated with mood and emotions, provided useful signals—an observation consistent with existing scientific literature. However, no single brain region, taken alone, yielded information clear enough to serve as a biomarker.
Important negative results
Even though these results discourage the use of structural MRI for depression screening, they provide valuable information.
Indeed, the prospect that artificial intelligence could identify mental disorders from brain scans is attracting growing interest. This study suggests that there are important limits to this approach—at least when restricted to current MRI methods and analyses of grey-matter structure.
The researchers estimate that their technique explains only about 6% of the variability in depression risk. This means that even with larger-scale studies, the predictive accuracy of structural MRI will likely remain limited.
We should not conclude that structural MRI is useless. It helps us understand the biology of depression and identify genetic and environmental factors that may affect the brain. However, if we want better predictions, we will need to explore other approaches.
Even if depression does not appear to leave a clear imprint in grey matter, other techniques—such as diffusion MRI to measure white-matter integrity or functional MRI to analyse brain activity—may help us capture the signature of the disorder from different angles.
A research tool, not a diagnostic test
Currently, the diagnosis of depression relies entirely on clinical evaluation.
However, studies of this kind help researchers better understand how genetic, developmental and metabolic factors interact with patients’ life experiences, shaping depressive episodes.
Grey matter is dynamic; its structure evolves throughout life depending on age, disease, or environmental exposures.
“In this study, we conducted what is known as a cross-sectional analysis, which means observing a population at a single point in time. For this purpose, we used only one MRI scan per individual. However, among the people studied, some had experienced depressive episodes several years before the imaging examination. To better capture how grey matter evolves and understand how it changes during and after a depressive episode, longitudinal data would be needed—that is, analyses of repeated MRI scans over a long period. Such data are not currently available at large scale, but represent a promising direction for future research,” the researcher concludes.
By setting realistic expectations and identifying the limits of current technology, the team hopes to guide future research toward more effective ways to study—and ultimately treat—depression.
[1] Global, regional, and national burden of disorders affecting the nervous system, 1990–2021: a systematic analysis for the Global Burden of Disease Study, The Lancet Neurology, 2021, mis à jour en 2024. https://www.thelancet.com/journals/laneur/article/PIIS1474-4422(24)00038-3
Sources
Jiang, J-C., et al. Applying machine-learning and deep-learning to predict depression from brain MRI and identify depression-related brain biology. Translational Psychiatry, Février 2026. DOI: 10.1038/s41398-026-03889-8.
Funding
This work was funded by the French National Research Agency, the European Union’s Horizon Europe programme, and Inria.
Image
Credit: Adobe Stock.

The ARAMIS team, led by Ninon BURGOS & Olivier COLLIOT, aims to build numerical models of brain diseases, particularly neurodegenerative pathologies, from multimodal patient databases. The main approaches used are machine learning (artificial...
Read more
Depression
Mental health, an essential component of our overall health, is a state of well-being, and an ability of the mind to function normally and respond appropriately to environmental stimuli. Mental disorders occur when this state of well-being is...
Read more